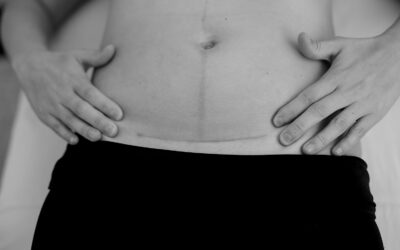
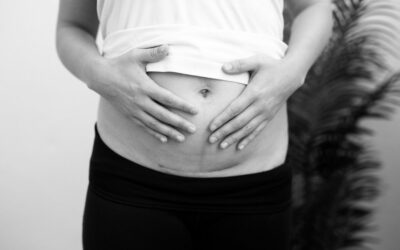
A topic often under-discussed is how breastfeeding or pumping affects your pelvic health and how estrogen plays into it. I want to shed some light on changes after childbirth and how breastfeeding or pumping affects your pelvic health.
During pregnancy, you have almost 30 times as much estrogen!
Hence, the occasional emotional outbursts! This increased estrogen plays a significant role in your baby’s development and your milk duct system. This is in preparation for breast milk production.
Immediately following childbirth, your estrogen levels drop drastically, allowing for an increase in prolactin. This is the primary hormone responsible for breast milk production. However, as you continue to produce breast milk, your prolactin levels stay high, and estrogen levels remain low, which can unexpectedly affect your pelvic health.
How do low estrogen levels affect your pelvic health?
When lactating, estrogen levels in your body decrease, and prolactin, the primary hormone responsible for breast milk production, increases.
Vaginal dryness
Within a few weeks after childbirth, your vagina can feel very dry, like a Sahara desert. It can stay this way as long as you produce breast milk. Vaginal dryness can cause discomfort wearing underwear or tight pants and contribute to pain with sex. Use a water-soluble lubricant during sexual activity to minimize friction, and work with a pelvic health PT if pain persists.
Lack of a period
Decreased estrogen may cause your postpartum period to not return for quite some time. If you breastfeed for only a short period, your period may return within 6-8 weeks after childbirth. But if you breastfeed or pump for an extended period, your period can take anywhere from 6-9 months to return or not until you completely stop breastfeeding, which may be over a year.
Lack of libido
Decreased estrogen levels during breastfeeding and pumping can also decrease sex drive. Returning to sex after having a baby entails a complex orchestra of factors. Sleep deprivation, leaking breasts, body image, pain, and parental responsibility all play a role in why the frequency of sex may decline after childbirth. No interest in sex postpartum is typical, so be kind and patient with yourself and return when ready.
Pelvic floor weakness
Lower estrogen levels contribute to thin vaginal tissues that may not be as supportive as before pregnancy. Take your time to return to exercise and high-impact activity. Your body has been through a significant transformation. It needs to heal, and your pelvic floor and core need to be rehabbed.
How to increase estrogen levels during breastfeeding
Foods that can naturally increase estrogen are those you’d find in a plant-based diet. You can also consider vitamins and minerals to boost estrogen. For example, consider soy products and those with phytoestrogens, such as the ones below.
- Legumes – lentils and beans
- Garlic oil
- Nuts and seeds
- Flaxseeds and sesame seeds
- Soy-miso and tofu
- Fruits – dried fruits and oranges, strawberries and peaches
- Vegetables – kale, sprouts, celery
- Dark chocolate
What can I do for pelvic health during breastfeeding?
#1 Get support
Work with a lactation consultant to guide you through latching, feeding, milk supply issues, and using a breast pump to help minimize stress and promote optimal rest and recovery postpartum.
#2 Moisturize, moisturize, moisturize!
Prick a small capsule of Vitamin E and apply oil to your labia and vaginal opening several times a day. Using a water-soluble lubricant can decrease friction during intercourse. Your physician or midwife may also recommend an estrogen-based cream, but this may affect your breastmilk supply, so speak to your healthcare provider about possible side effects.
If pain with intercourse persists after these remedies, work with a pelvic health physical therapist for muscle relaxation and tissue softening to help decrease pain and sensitivity.
#3 Switch up your period products
Your postpartum period may have a heavier flow than pre-pregnancy and require changes to your menstrual care routine. Consider using a menstrual cup for a heavier flow, switching to pads and liners if tampons do not comfortably stay inserted, and using organic, nontoxic products for sensitive vaginal and vulvar tissues.
Remember, these changes are only temporary.
The effects of breastfeeding on your pelvic health are short-term and will all improve as milk production decreases and your feedings become less frequent. Breastfeeding will also not have any long-term effects on urinary leakage or pelvic organ prolapse, as research found no increased risk of these symptoms in exclusively breastfed women. Your breastfeeding journey may last a few days or several years – it is an individual experience for everyone.
If you’re interested in some additional support during this time, check out the V-Hive membership’s postpartum program. With short, at home exercises you’ll be guided through a 12-week program to help strengthen your pelvic floor and core post baby.