When discussing injuries sustained during childbirth, there is a lot of discussion about perineal tearing, prolapse, and diastasis recti. While these injuries are certainly cause for discussion, there’s a lesser known but fairly common birth injury we rarely hear about, and that’s pelvic floor avulsion tears. So what is a pelvic floor avulsion tear? Pelvic floor avulsion tears occur when a portion of the pelvic floor muscles tear away from the bone during childbirth.
While these tears are fairly common, they are often difficult to diagnose as they are not a tear that can be visualized during a routine postpartum assessment. While diagnosis can be obtained through ultrasound and/or MRI, patients often do not recognize symptoms until much later, making diagnosis and treatment difficult. Proper diagnosis and treatment also require a good understanding of the pathophysiology of the injury by the physician.
What exactly is torn?
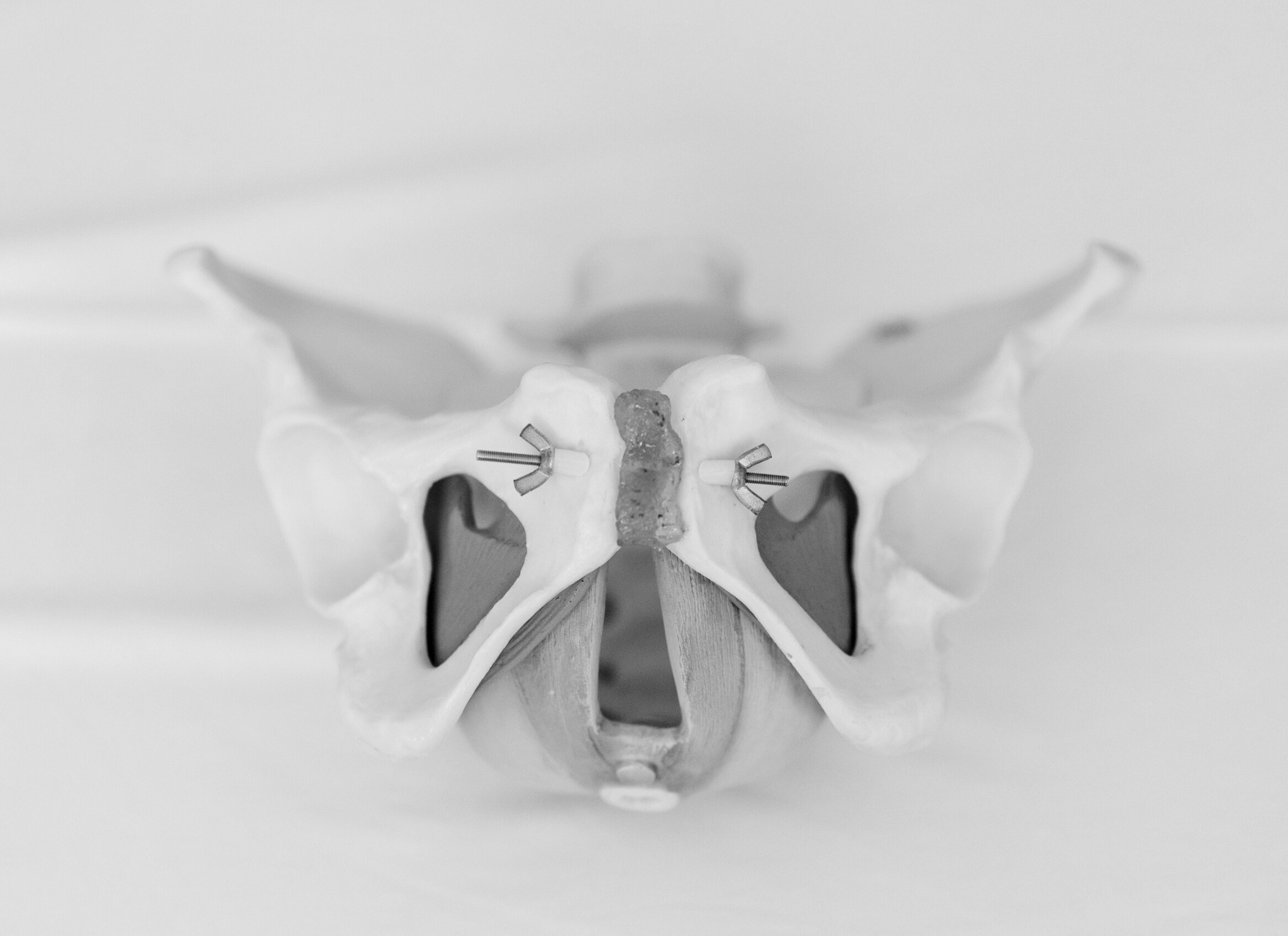
To understand pelvic floor avulsion tears, first we must understand the anatomy of the structures involved.
Pelvic floor avulsions most commonly occur in the levator ani muscles of the pelvic floor. This muscle group, which includes the puborectalis, the pubococcygeus, and the iliococcygeus, make up the deep layer of the pelvic floor.
The levator ani, in addition to the connective tissue around it form what is called the pelvic diaphragm. The pelvic diaphragm is predominantly responsible for postural support of the abdominal and pelvic organs, and plays a significant role in bowel and bladder function.
How does this happen and what are the risk factors?
During childbirth, these muscles have to stretch considerably in order to allow the baby to pass through the vaginal canal. Studies have found that these muscles can stretch to 3x their normal length in some women during delivery.
Needless to say, stretching to that extent puts a lot of strain on those muscles and in some cases may lead to tearing. Avulsion tears have been found to occur in 10-36% of women, and most frequently occur in forceps assisted deliveries. While forceps delivery is the most distinct risk factor, other risk factors for avulsion tear include:
- An occiput posterior positioned (or sunny side up) baby
- A baby with an exceptionally high birth weight and larger fetal head circumference
- Vacuum-assisted delivery
- Maternal age greater than 33
- A longer second (pushing) stage of labor
What does this look like?
It is important to note the symptoms a patient might experience, as well as the risk factors. Knowing both can help with early identification and diagnosis of an avulsion tear. This early identification will lead to early intervention, and will ultimately reduce the possibility of further pelvic floor dysfunction. Some symptoms reported and clinical findings of patients with levator ani tears include:
- Pelvic heaviness or pressure (Do you feel like your insides are falling out?). This is often worse at the end of the day or during/immediately after exercise.
- Decreased sexual desire, arousal, or ability or orgasm
- Limited sensory awareness
- Vaginal wall laxity
- Pelvic floor muscle weakness (may present as one sided weakness if the avulsion tear is unilateral)
While subjective reporting is an important part of diagnosis, definitive diagnosis is often obtained through a combination of pelvic exam/palpation, measurement of the genital hiatus (space from the urethra to the perineum), ultrasound, and MRI.
A diagnosis of levator ani avulsion tear will ultimately come from your physician, but pelvic PTs often play an important role in early detection, and can be an advocate for the patient to receive further diagnostic testing through communication with or referral to the physician. Therefore, it is important for pelvic PTs to be well versed in the signs, symptoms, and clinical findings of a patient with levator ani avulsion tear.
You’ve seen your MD, and you’ve gotten a diagnosis… now what?
Although surgical repair can be done, there is little research on the use of surgical repair to treat a levator ani tear. Thankfully, this diagnosis is beginning to gain recognition in the pelvic health world, and therefore we are likely to see much more research in the near future. Despite the lack of research at this time, there are factors to consider when discussing surgical repair. Those factors include:
- The extent of the tissue injury
- The length of time passed since the initial injury
- Any history of prior birth injury or pelvic trauma
- Contributing factors that might reduce the success of the surgery
- If the patient had physical therapy to address any factors that may reduce the chances for a successful surgery
- The experience of the physician performing the surgery and the facility at which the procedure will be done
- Ultimately, if you are considering surgery you’ll want to choose a surgeon who has experience with levator ani repair, who understands any and all activity you would like to return to, and who will work closely with a pelvic PT before and after surgery to ensure the best possible outcome. You’ll also want to make sure you’ve discussed all possible treatment options prior to undergoing surgery.
Help! My avulsion tear went undiagnosed!
When left untreated, these tears can lead to many forms of pelvic floor dysfunction including pelvic floor muscle weakness, urinary incontinence, pelvic organ prolapse, chronic pelvic pain, pain with intercourse, low back or hip pain, and limited function with desired exercise or daily activity.
One of the most common, long term complications from an avulsion tear is the development of pelvic organ prolapse (2x more likely to have bladder prolapse and 3x more likely to have uterine prolapse). This typically occurs over time and not right away. One study even found that the average timeframe of diagnosis for avulsion tears was 33 years post delivery.
Therefore, women who go undiagnosed for an avulsion tear will likely experience more significant grades of prolapse than those who are diagnosed and treated promptly.
This is because the muscular structures meant to support their pelvic organs (the levator ani) are no longer intact and therefore unable to provide adequate support during daily activity and exercise. Without proper treatment (pelvic PT, surgery, activity modification, or a combination) the tissues continue to be taxed past their capabilities and the prolapse becomes worse.
So what do we do when diagnosis is delayed and prolapse has already begun to occur?
Have no fear, pelvic PT is here!
The great news is that even if you went undiagnosed for an avulsion tear and have developed pelvic organ prolapse, pelvic PT can help! Some of the ways in which a pelvic PT can help include:
- A thorough pelvic exam to assess remaining muscle strength, length, endurance and motor control.
- An assessment of your prolapse lying down and in standing to determine how well you are managing the stresses on your pelvic floor.
- Real time feedback on the quality of your pelvic floor contraction to help improve function of your pelvic floor muscles, and support to your organs.
- Determining if you may benefit from an external supportive device like a pessary.
- Personally fit you for a pessary or refer you to a provider who can if they cannot.
- Teach you pressure management strategies to reduce any unwanted stress on your tissues with daily activity or exercise.
- Provide guidance on how to safely continue your desired exercise without further injury to your tissues.
Some of the main pressure management strategies your PT may recommend include:
- Use of a squatty potty or small stool with bowel and bladder emptying.
- Avoid excessive straining or breath holding for bowel movements.
- Avoid peeing just in case, or “power peeing.”
- Use of a slow exhale and pelvic floor activation with exertion (lifting, coughing, sneezing, exercise).
- Balancing high level activities (running, lifting, HIIT) with mobility work (yoga, stretching, foam rolling).
- Modifying any activity that causes pelvic heaviness, or pressure, a sensation that your insides are falling out, stress urinary incontinence, or low back pain.
So if you are experiencing any of these symptoms, I urge you to speak with your pelvic PT and/or OB. They can help get the ball rolling on diagnosis, begin treatment, and refer you out to a urogynecologist if need be. If you’re local to New Orleans, please come see us at NOLA Pelvic Health. If non-local, don’t forget we offer virtual consultations. We would love to help!
*Articles referenced in this post can be found here, here and here.
___________________________________________________________________________________________
Interested in more tips on how to prevent or overcome Pelvic Floor Problems?
Download this free guide for some simple, do-able, totally-not-weird tips to take better care of your down there.
___________________________________________________________________________________________
Some links may be affiliates. This means we may make a small commission if you make a purchase. The products we recommend on this website and in blog posts are always products we use ourselves or recommend to clients. Thank you for supporting us in our mission to revolutionize women’s healthcare.