During the first weeks postpartum, my baby was inconsolable. And something didn’t feel right. I didn’t know if I was terrible at parenting, bad at breastfeeding, or bad at reading my baby’s cues. It was overwhelming. Turns out my baby wasn’t getting enough food.
Luckily, I could reach out to my midwives regularly via text, phone calls, and home visits. I expressed my concerns, and they listened and offered advice. But unfortunately, the early intervention made us realize that I wasn’t producing much milk yet. It’s normal for milk to take a few days to come in, but this was different – I may not have the potential to produce much. I have something called tubular breast deformity, or tubular breasts.
What is Tubular Breast Deformity?
Even working in healthcare, I had never heard of this diagnosis before. Though this condition isn’t considered rare, it is unique. Women often don’t seek treatment. The condition is also known as tuberous breasts, breast hypoplasia, or hypoplastic breasts.
What are the Signs of Tubular Breasts?
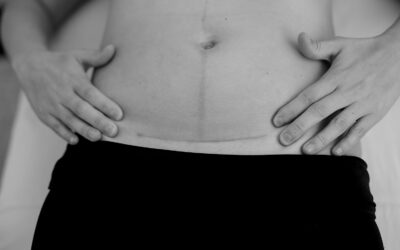
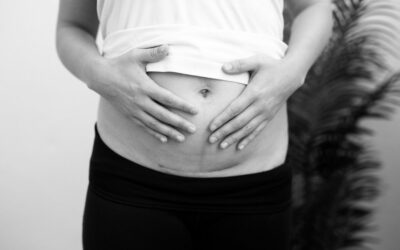
- Tubular breasts (like diastasis recti) often have a gap in them – 1.5 inches or more is the standard measurement for diagnosis.
- Tubular breasts are often different sizes, with one breast being larger.
- The breasts may look “collapsed.”
- The areola is often quite large – larger than average.
How do you Know if You Have Tubular Breasts?
If you have any of the above, make an appointment with your healthcare provider. You’ll want to find one who has knowledge of and experience with this condition, as it’s not widely known or diagnosed.
Can Tubular Breasts Go Away?
Tubular breasts won’t go away on their own or through lifestyle changes. Surgery is often needed to correct this condition through breast augmentation. Fat grafting is another option and is slightly less invasive than breast augmentation. This is a cosmetic procedure performed by a plastic surgeon.
Can Tubular Breasts Produce Milk?
Breastfeeding will be difficult (more than it already is) if you have this condition. In addition, due to the lack of glandular tissue (the tissue that produces milk), producing milk will be hard. For me, my baby was latching well, and it wasn’t that I wasn’t producing anything, but it wasn’t enough to fill her up. She was sucking so much that it burned many calories while not getting enough. I was lucky enough to have a friend willing to share a week’s worth of breast milk with me so I could keep giving her breast milk while I navigated this new obstacle.
Trial Pumping
For my journey, I started trial pumping while still breastfeeding some. Then I tried exclusive pumping around the clock, every 2 hours, including overnight, to stimulate production. I slept in a different room the first night I tried this and set alarms every 2 hours: wake up, pump, attempt to syringe out any teeny tiny bit of milk to save for Rowan, rinse the pump and charge it, then back to bed, only to wake up roughly an hour later and repeat. Rowan was being bottle-fed the donor milk from my husband during the night.
After just two nights of this, it didn’t feel right to me. It was hard. I wasn’t sleeping, and you need sleep and relaxation to produce well. There was a desire to be near my baby and my husband. So I loosened up on the pumping regularity and decided just to pump when Rowan woke up to eat. I would pump, and my husband would feed her.
But this strategy was also really hard on us. Both of us woke up at the same time. We lost precious sleep that we could be trading off or more relaxed during. I also tried various foods, drinks, teas, and other herbal remedies, which all cost money.
Is it the Pump?
Then I started to question my actual pump. I chose to use the Elvie pump, a hands-free mobile pump. You cannot see how much you’re pumping in real time due to the pump being inside the bra. So I wouldn’t know until the end of the session if I got anything. It’s supposed to tell you on your phone app how much you’re producing, but mine was not always accurate at such small amounts.
My midwives were able to lend me a hospital-grade pump, and for better or worse, my results were about the same. I tried to up my pumping frequency again, but I was mentally shot. My husband went back to work on day four and I was taking care of Rowan all day by myself. It was hard to attempt to pump with a hands-free pump while caring for/feeding/holding Rowan. She didn’t sleep much during the day at this point. It was near impossible to care for her while pumping.
Using Donor Breast Milk
When the first week of donor breast milk was out, a fantastic anonymous mama donated some breast milk to my midwives, who shared that with me/Rowan. This was a relief because, during this time, I was still really stuck on staying with breastmilk as long as possible. All the breastfeeding books brainwashed me not to try formula yet, but also during this time, Rowan started to have gas/upset stomach issues. Her cry was intense and painful to hear, and I wasn’t sure if it could be a reaction to something in the diet of the breast milk donor mother. Many friends have shared their kiddos had difficulty digesting certain foods through breast milk, such as dairy, broccoli, spicy foods, etc. So I had some difficult decisions to consider going forward.
Switching to Formula
Ultimately I hit a point where I was ready to switch to formula as her primary source of food. I was prepared to let go of donor milk’s uncertainty, breastfeeding and pumping. I don’t feel like I gave up. Instead, I feel like I gave it a decent try, and in the end, it’s not what was going to work best for the happiness and health of our family.
After attempting to pump exclusively for more than a week, there was a moment when Rowan was fussy, and I tried to calm her by breastfeeding. Unfortunately, it didn’t go as smoothly as previously, and I knew it was my last time breastfeeding her. Something I had looked forward to doing to provide for her was over. But at the same time, I felt at peace with my switch to formula, and a huge weight was lifted. I mean huge. Calmness came over all of us—our entire family.
Making Peace
I feel so privileged I was able to take the time to research formulas. In the end:
- I chose HiPP (dutch version).
- I’m grateful I have the financial resources to provide my baby with high-quality formula.
- I’m thankful for the donor milk she was able to eat while we worked on making this decision and exhausting milk production possibilities.
- I’m grateful we were able to experience some breastfeeding.
I probably only breastfed up until weeks 2-3 and pumped until week 4. I’m unsure of the exact dates because I was in quite a fog. But when we made the switch to a consistent formula, wow. The baby was fed. The baby started sleeping better and I felt I could parent better. The time previously spent devoted to pumping I could now use for being there for my baby, myself, and my partner. I was sleeping and I could breathe again.
Every Breastfeeding Journey is Different
I’m so in awe of the mamas who commit to breastfeeding and pumping, who work through struggles of latching, overproduction, and underproduction. Who find ways to fit this in to provide for their baby. But I also have whole new respect for mamas who know this road is not for them, whether by choice or not.
I had a friend who shared with me during this time that she hated breastfeeding and instead exclusively pumped. And yet another friend who shared that she couldn’t stand pumping or breastfeeding and hated every minute of it. This honesty helped me cope. Yes, breastfeeding has many incredible benefits. Our bodies are magical. But it is essential that your baby gets fed and that you feel healthy. Whatever decision feels right for you, explore it and own it. I read multiple breastfeeding books before birth, but I did not prepare for what formula I might want to use to supplement or switch to if things didn’t work out.
Fed is Best
As a planner, that is something I wish I had taken the time to do. I wish I would have felt okay with using the formula to supplement earlier while still attempting to breastfeed a small amount, as this may have put less pressure on me. Being able to feed my baby was a rollercoaster of emotions. I put so much pressure on myself. And I had a lot of healing to do about not being able to supply her with my milk. I had a lot of healing to do in loving my body. There are many reasons why someone may choose (or not have a choice) how they feed their baby. Let’s support one another in all our journeys.
Some links may be affiliates. This means we may make a small commission if you make a purchase. The products we recommend on this website and in blog posts are always products we use ourselves or recommend to clients. Thank you for supporting us in our mission to revolutionize women’s healthcare.