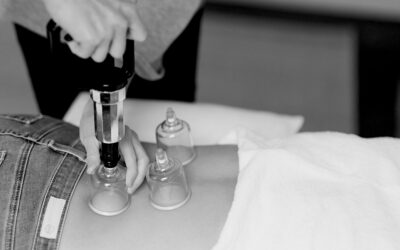
What does prolapse feel like? Wondering if you have it? Being diagnosed with pelvic organ prolapse can feel overwhelming. You may feel like you can’t so much as sneeze without risking feeling vaginal pressure. You may not know what can even help.
There is little guidance, and Dr. Google is far from reassuring. But the good news is that not all prolapse diagnoses are equal. Often, prolapse is treatable without surgery. It is likely you can improve your prolapse as well. But to know how to treat prolapse, we first have to understand what it is.
What is pelvic organ prolapse?
There are different types of prolapse. It occurs when connective tissue that normally holds these organs in place weakens or stretches over time. Uterine prolapse is a condition in which the uterus descends in the pelvic cavity. Pelvic organ prolapse causes one or more of the pelvic organs to drop down into the walls of the vagina. This happens one of three ways:
- Anteriorly: from the bladder or urethra
- Posteriorly: from the rectum or intestines
- Apically: from the cervix or cuff scar after a hysterectomy
What does prolapse feel like?
What does prolapse feel like? POP can cause a variety of symptoms including discomfort during intercourse and chronic cough due to strain on the diaphragm. Pelvic organ prolapse may feel like:
- Vaginal pressure or bulging (like something is trying to bulge out of the vagina)
- Feeling that your insides are falling out of your vagina
- Low back pain that is worse as the day goes on
- Pelvic heaviness that is worse at the end of the day
- Difficulty emptying when peeing or pooping
- A need to re-position during poops
- Urinary leakage
The stages of prolapse
There are also varying stages or degrees of prolapse. Pelvic organ prolapse quantification (POP-Q) is a tool used to measure the degree of pelvic organ prolapse. It measures the location, descent and size of the bladder, uterus and rectum. It does this using standardized points relative to the hymen or anterior commissure.
The grades of prolapse range from 0 (not present) to 4 (full eversion or lowering of the tissue). Stage 4 occurs when the organ involved is actually protruding out of the vaginal opening. This needs surgical intervention. You can treat Grades 1 through grade 3 with physical therapy and supportive devices. PT addresses the causative factors that lead to prolapse. PT can help you strengthen your weakened vaginal wall.
Causes of prolapse
While pregnancy and delivery is one known cause, it is definitely not the only one. It is possible to have more than one risk factor, which will increase the likelihood of prolapse. Other causes of prolapse can include:
- Vaginal and/or vulvar trauma via vaginal deliveries
- Tissue restriction from healing cesarean scars or perineal scars
- Chronic pelvic floor muscle overactivity
- Hormonal changes during menopause
- Pelvic surgery
- Congenital factors
- Race (Caucasian women are at higher risk)
- Activities that increase pressure in the abdomen
- Improper breathing with weight lifting
- Chronic constipation
- Chronic obstructive airway disease
Where to start with treatment
There are many treatment options available. Before an internal assessment, your PT will take a thorough history. What does your day to day look like? Do you have a physically taxing job? What is your bowel and bladder function like? Do you have pain with intercourse? How many pregnancies and deliveries have you had, and was there any trauma? What does your exercise routine consist of?
These are all questions your pelvic PT should be asking you at your initial evaluation. Gathering this gives us an idea of the types of stresses your tissue are sustaining on a daily basis. This will help us determine the best treatment!
Kegels may not be appropriate
Prolapse often occurs due to inadequate pressure management with activity. Another reason is pelvic floor muscle overactivity with muscle inefficiency (weakness). Because of this, “doing your kegels” will likely not improve your symptoms and may even make them worse.
Other things you can do to help
Here is a list of some of the things we recommend for activity modification and treatment.
- Get a squatty potty! The squatty potty is not a gimmick. It actually works. Use the squatty potty to poop AND pee. This puts your pelvic floor muscles in a more lengthened position. Doing so will make pooping and peeing easier. This will reduce the likelihood of straining. Thus, reducing the pressure on the already weakened vaginal wall.
- A popular alternative seating solution to alleviate symptoms is sitting on a ball. Sitting on an exercise ball engages and strengthens core muscles, while providing support to the pelvic area.
- DO NOT PUSH THE PEE OUT! That’s right, straining to get the flow of urine going is not how you should pee. So, when you sit on the toilet, let the flow of urine begin on its own. The same applies to “just in case” peeing. You should only be peeing if you have true urgency. This same methodology applies to bowel movements as well.
- BREATHE! More exhales! When stressed, do you hold your breath? Or when something becomes physically challenging? Breath-holding can increase the pressure in your abdomen. It can also increase the pressure on the muscles of your pelvic floor and your vaginal wall. So, start using a slow exhale (like blowing out birthday candles) when you exert energy. This includes when working out, picking up kiddos or pets, at work if you have a physical job, etc).
- Drink that smoothie… through your vag. Draw in your lower abdomen and pelvic floor as if you were trying to sip a smoothie through a straw in your vagina. You want to engage your pelvic floor and lower abdomen (at the same as you exhale). By doing so, you are supporting the more vulnerable tissues of your vaginal wall.
- Be mindful of infections. Bladder infections are common in women with pelvic organ prolapse. These infections can cause pain and burning during urination, frequent urging to urinate, cloudy or bloody urine.
Modify and stretch
Modify any activity that causes:
- Increased pelvic area heaviness or pressure
- Urine leakage
- Pelvic or low back pain
- Protruding of your tissues out of the vaginal opening
Find a balance between lengthening any overactive pelvic floor muscles and retraining them. You want to improve their strength and motor control. Always incorporate activities that improve pelvic floor relaxation (walking, gentle yoga, stretching). This is important if you do HIIT (Orange Theory, Crossfit, powerlifting, Pilates, competitive sports or running).
- Find stretches that help including:
- Child’s pose
- Knee to chest stretch
- Butterfly
- Pigeon
- Deep squat
- Piriformis stretch
- Cossack squat
- Spiderman lunge
Stretch before AND after high intensity activity.
Performing stretches prior to working out can help address any tightness present before you begin your workout, which ensures proper muscle function during the workout.
Knee to Chest
Sit on the floor with your feet flat on the ground. Inhale deeply and, as you exhale, bring one of your knees up towards your chest. Wrap your hands around the back of the thigh to pull your knee in closer and hold the position for 15 to 20 seconds.
Child’s pose
Start by kneeling on the floor with your knees hip-width apart. Keep your big toes touching each other and sit back onto your heels. Then, bring your chest towards the floor and rest your forehead on the ground. Reach forward with your hands and spread your palms out flat onto the floor in front of you. Hold this position for 30 seconds to a minute before slowly coming back up into kneeling position.
Pain and symptom management options
External support devices include:
- Bao Bei maternity support leggings, shorts, or bloomers
- SRC compression shorts or leggings
- V2 Pelvic Floor press
Internal Supportive devices include:
- Poise Impressa (order the sizing kit first to determine appropriate size)
- Pessary (you’ll need an OB/GYN or Urogynecologist to fit you)
- A regular tampon (use a tampon for added support with exercise)
- Pelvic elevation at the end of the day. Use a pelvic wedge or place pillows under your pelvis (as shown below). This can help reduce swelling and pressure in the vulvar and vaginal regions. Use this with a heating pad on your low back if you also have low back pain. You can also put ice on your pelvic floor if you have a lot of vaginal or vulvar pain. We recommend you do this for about 10 minutes per day.
- Work with a Pelvic Health Physical Therapist. We offer online sessions and in-person sessions to help!
Pelvic organ prolapse and pelvic floor disorders are important health issues that can have a significant impact on an individual’s quality of life. You may be wondering if your prolapse will feel like this forever. It’s important to get the help you need. Contact us or your local physical therapy office to get the care you need.
___________________________________________________________________________________________
Interested in more tips on how to prevent or overcome Pelvic Floor Problems? Download this free guide! You’ll get simple, do-able, totally-not-weird tips to take better care of your down there.
Some links may be affiliate links. The products we recommend are products we use or recommend to clients
___________________________________________________________________________________________